Blog at a glance
-
Postmenopausal bleeding is any vaginal bleeding after 12 months without periods
-
The pattern of bleeding can vary from person to person
-
Common causes include tissue thinning, hormone therapy, polyps, and other conditions like uterine cancer
-
In many cases, the cause is simple and manageable
-
The amount of bleeding does not always indicate what’s happening
-
Any bleeding after menopause should be evaluated by a healthcare provider

Bleeding After Menopause: What It Means, Common Causes & When to See a Doctor
As women move into midlife, the body naturally goes through changes associated with menopause. This is a normal phase of life, but it can bring symptoms that feel new, unfamiliar, or sometimes concerning.
In the United States, millions of women experience menopause each year, and up to 80% of women report symptoms such as hot flashes, sleep changes, or shifts in their usual patterns. While many of these symptoms are manageable, they are not always well understood.
In many cases, women are unsure about what is expected and what is not. This lack of clarity can lead to hesitation, some may ignore symptoms, while others may feel worried but unsure whether they need medical attention.

One situation where this uncertainty becomes especially important is bleeding after menopause.
For many women, this can feel unexpected and raise immediate questions, whether it is something temporary, something to monitor, or something that needs attention. Because this stage of life is often associated with the end of menstrual cycles, any new bleeding can feel confusing.
The important thing to understand is that while many causes are simple and manageable, bleeding after menopause should be evaluated to understand the cause.
This guide is designed to bring clarity, helping you understand what bleeding after menopause may indicate, what patterns to pay attention to, and when it’s important to seek medical advice.
What is Considered Postmenopausal Bleeding?
Before looking at causes or concerns, it’s important to first understand what is actually considered bleeding after menopause.
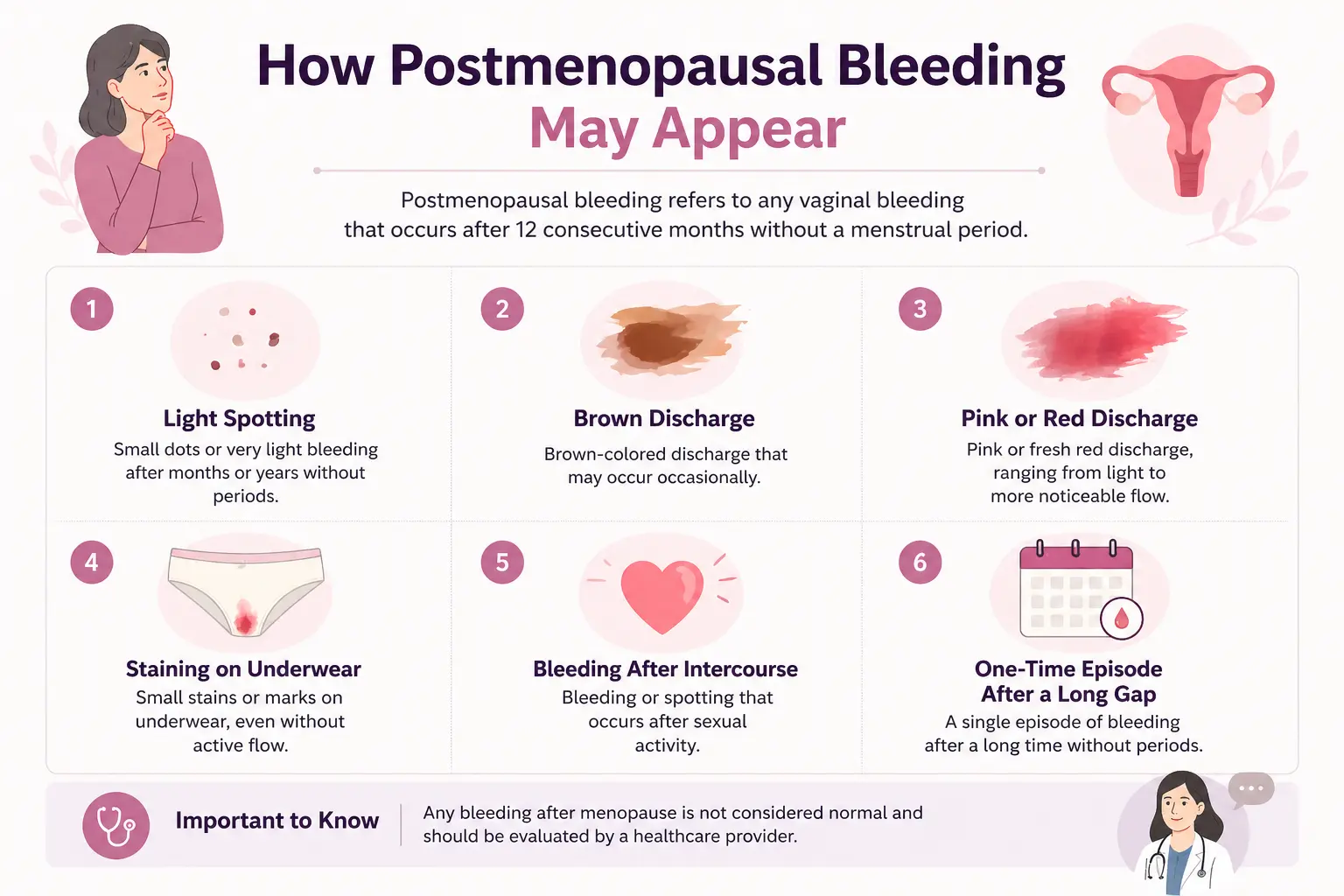
Postmenopausal bleeding refers to any vaginal bleeding that occurs after a woman has gone 12 consecutive months without a menstrual period.
After this stage, the body is no longer expected to have regular menstrual cycles. Because of this, any new episode of bleeding, whether light spotting or more noticeable flow, should be evaluated by a healthcare provider.
This may include:
-
Light spotting after months or years without periods
-
Brown, pink, or red discharge
-
Staining on underwear
-
Bleeding after intercourse
-
A one-time episode after a long gap
-
Bleeding that feels similar to a period
Common Question
Is bleeding after menopause normal?
No, bleeding after menopause is not considered a normal part of menopause. Once periods have stopped for 12 consecutive months, any new bleeding should be evaluated. At the same time, many causes are simple and manageable, especially when identified early.
Why am I bleeding after menopause?
Bleeding after menopause is usually linked to changes in the vaginal or uterine lining due to hormonal shifts. In many cases, the cause is not serious, but since different conditions can present in similar ways, it’s important to identify the exact reason.
Does the amount of bleeding matter?
The amount of bleeding does not always give a clear indication on its own. Even light spotting or a single episode can still need attention. What matters most is that it is happening after menopause, which is why any bleeding should be evaluated by a healthcare provider.
|
What Causes Bleeding After Menopause?
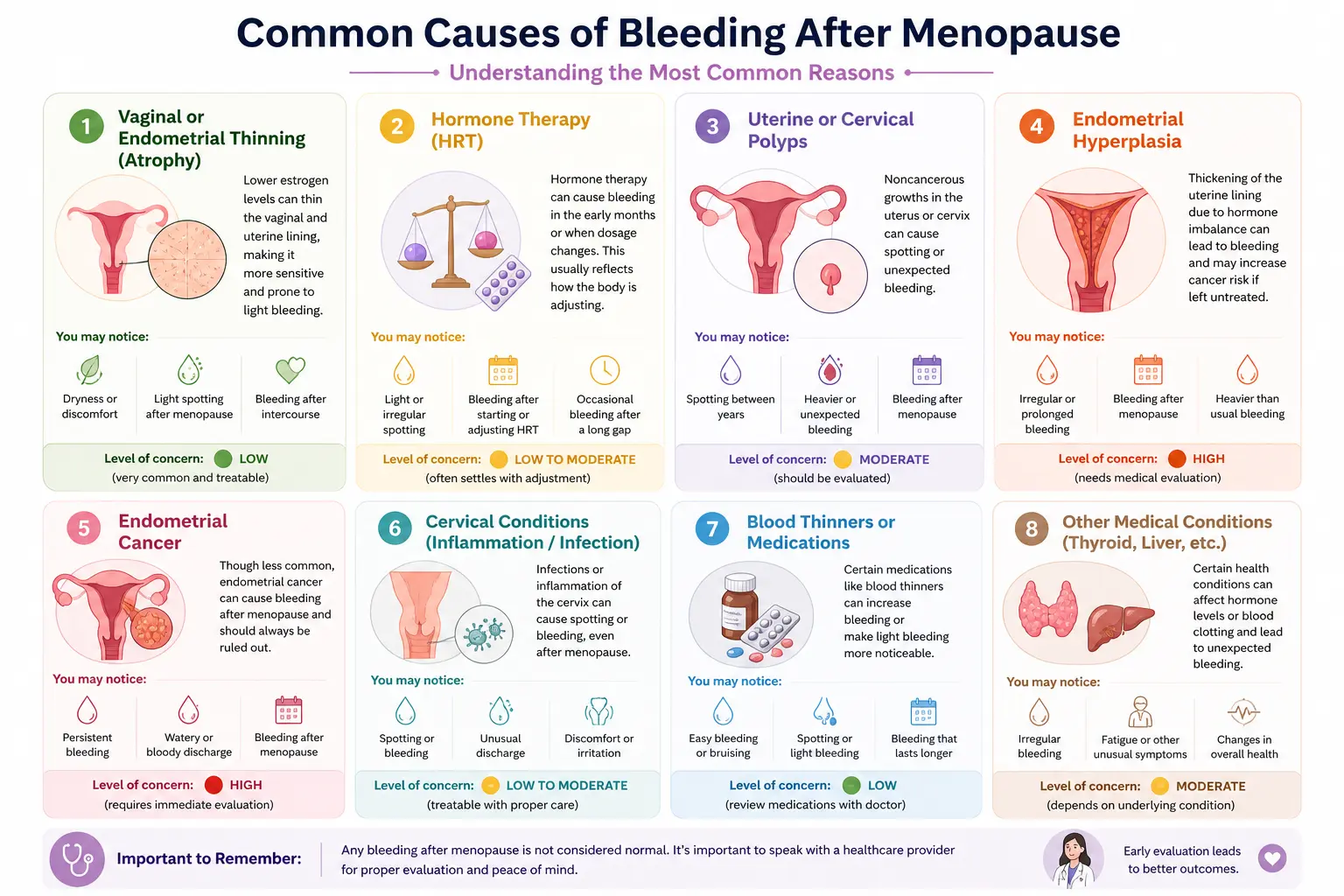
Bleeding after menopause can occur for several reasons, and in many cases, the cause is simple and manageable. While some conditions may need closer attention, most are not serious.
It’s also important to note that similar symptoms can have different causes, so identifying the exact reason helps guide the right approach.
1. Vaginal or Endometrial Thinning (Atrophy)
This is the most common cause of bleeding after menopause. Lower estrogen levels can make the vaginal and uterine lining thinner and more sensitive, which may lead to light bleeding with minor irritation.
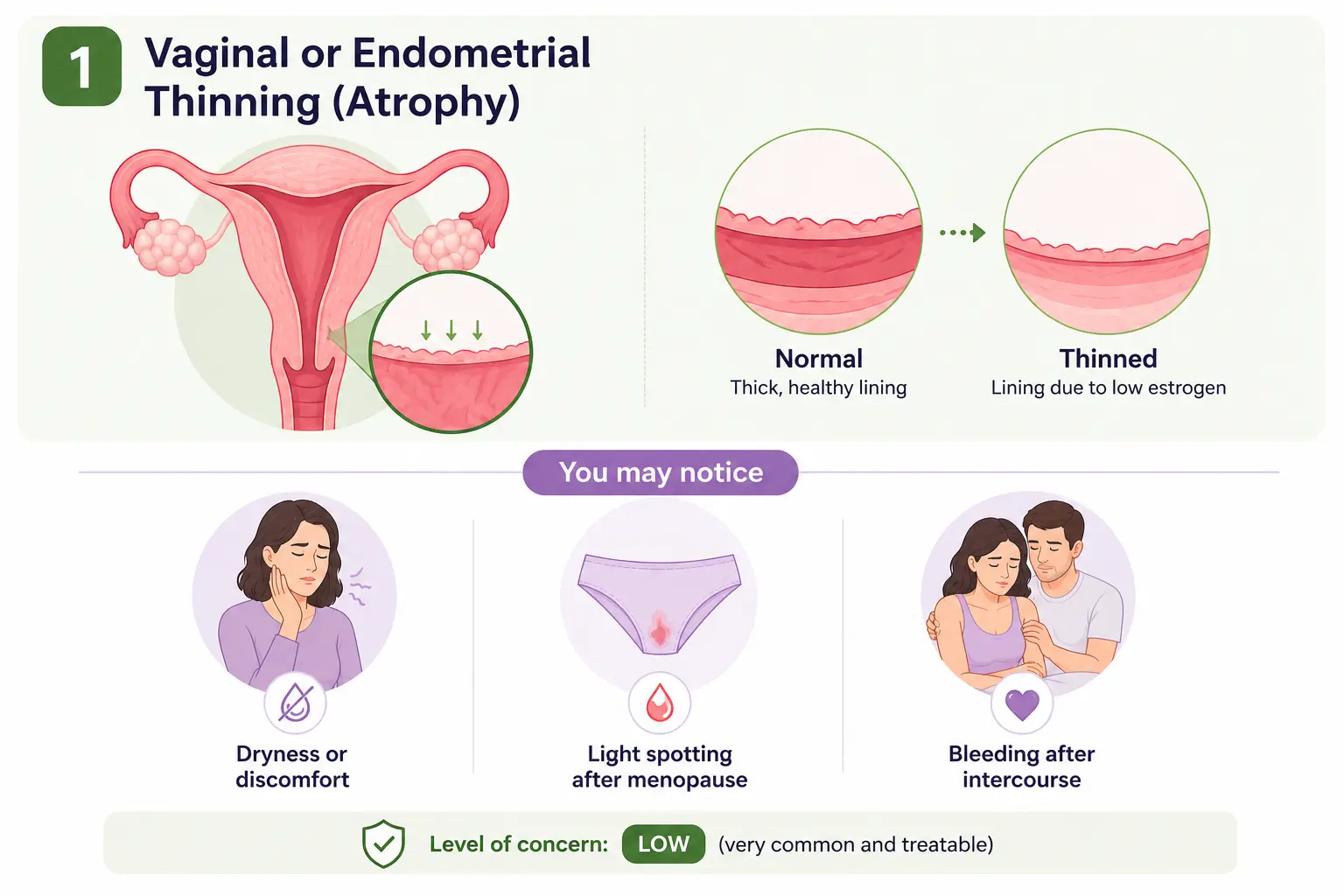
You may notice:
Level of concern: 🟢 Low (very common and treatable)
2. Hormone Therapy (HRT)
Hormone therapy can sometimes lead to bleeding after menopause, especially in the early months or when there are changes in dosage. This usually reflects how the body is adjusting to hormone levels.
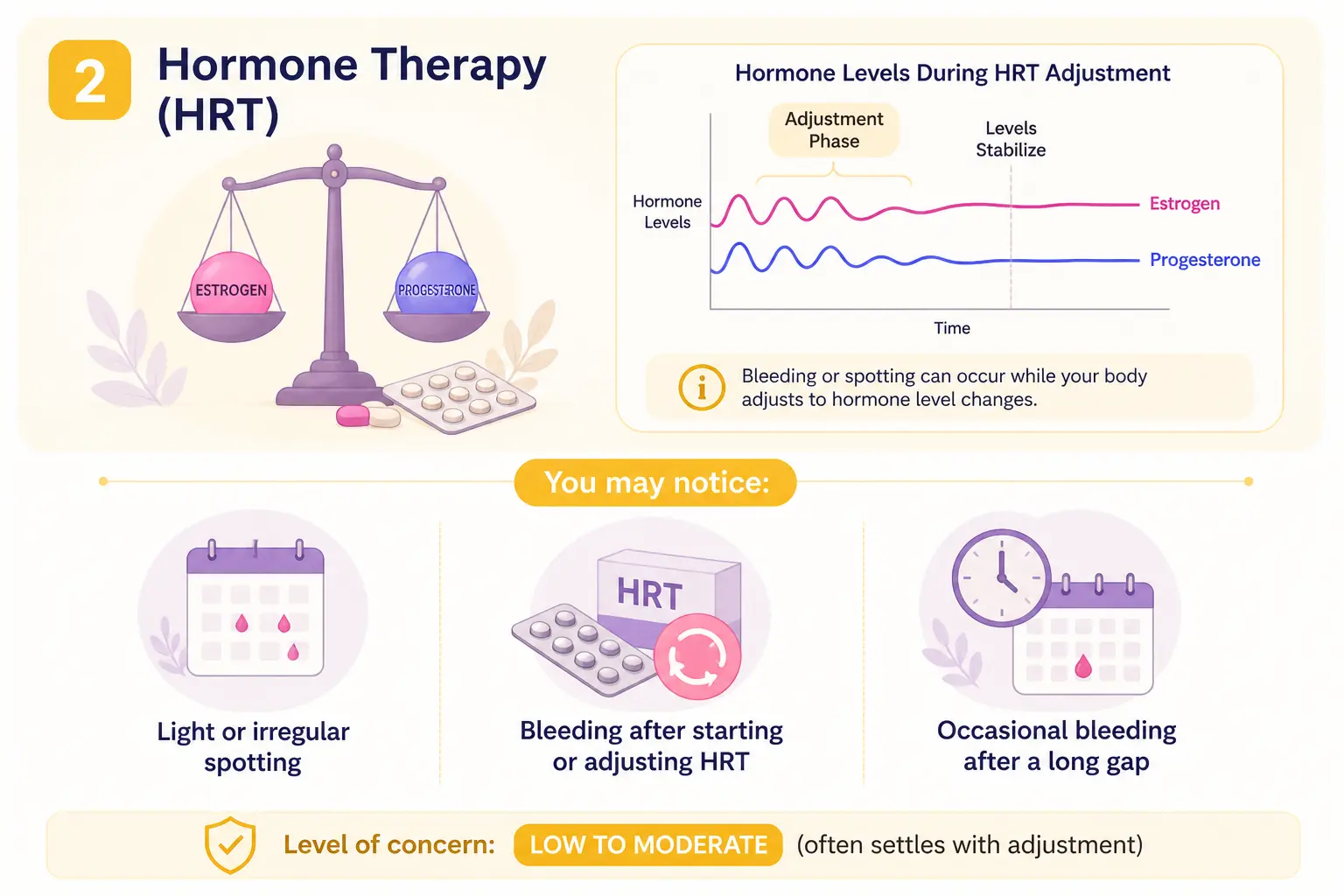
You may notice:
-
Light or irregular spotting
-
Bleeding after starting or adjusting HRT
-
Occasional bleeding after a long gap
Level of concern: 🟡 Low to Moderate (often settles with adjustment)
3. Uterine or Cervical Polyps
Polyps are small, usually non-cancerous growths in the uterus or cervix that can lead to bleeding after menopause or irregular spotting. They are relatively common and often easy to treat.
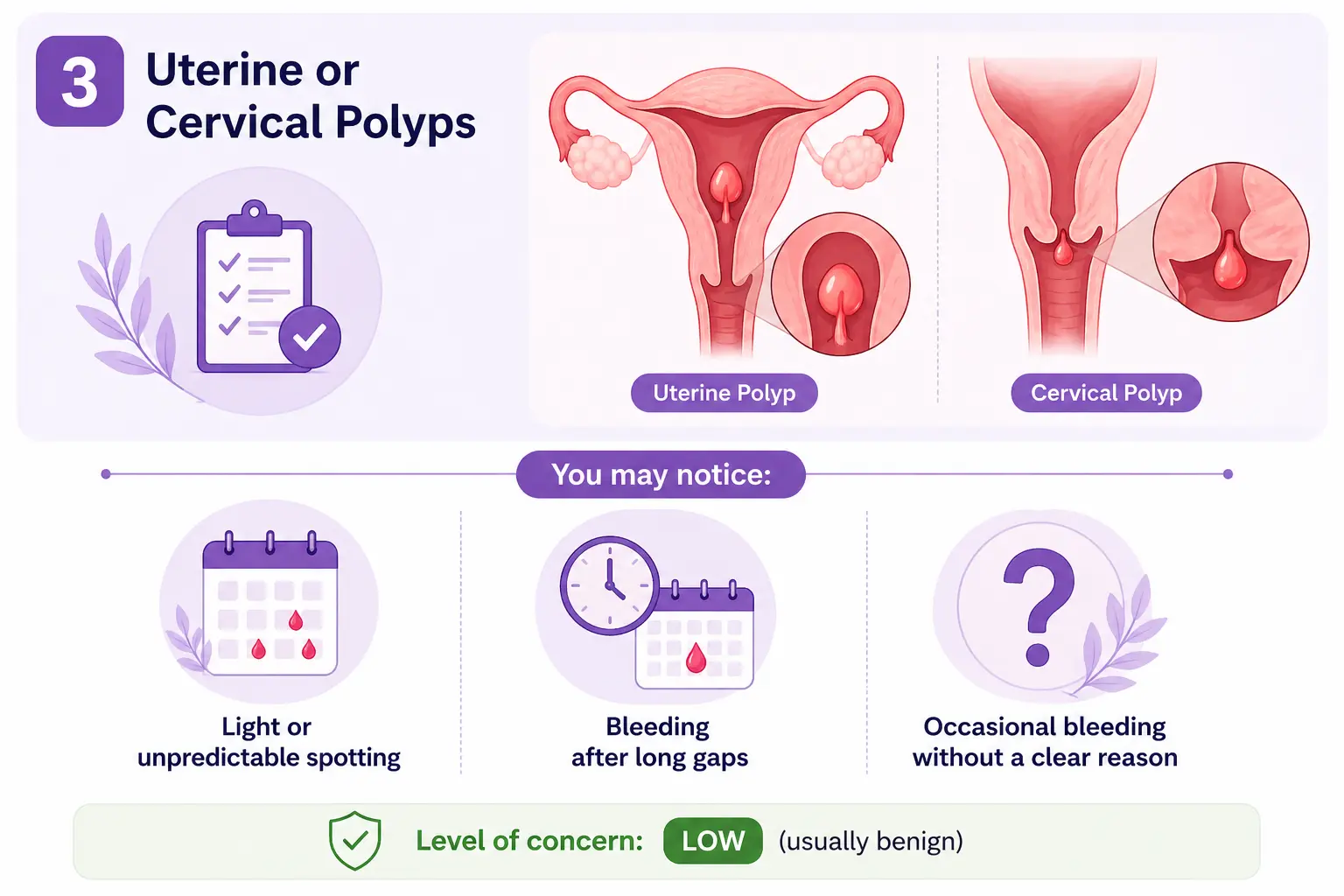
You may notice:
Level of concern: 🟢 Low (usually benign)
4. Endometrial Hyperplasia
Endometrial hyperplasia refers to a thickening of the uterine lining, often related to hormonal imbalance. In some cases, it may require treatment to prevent further changes.
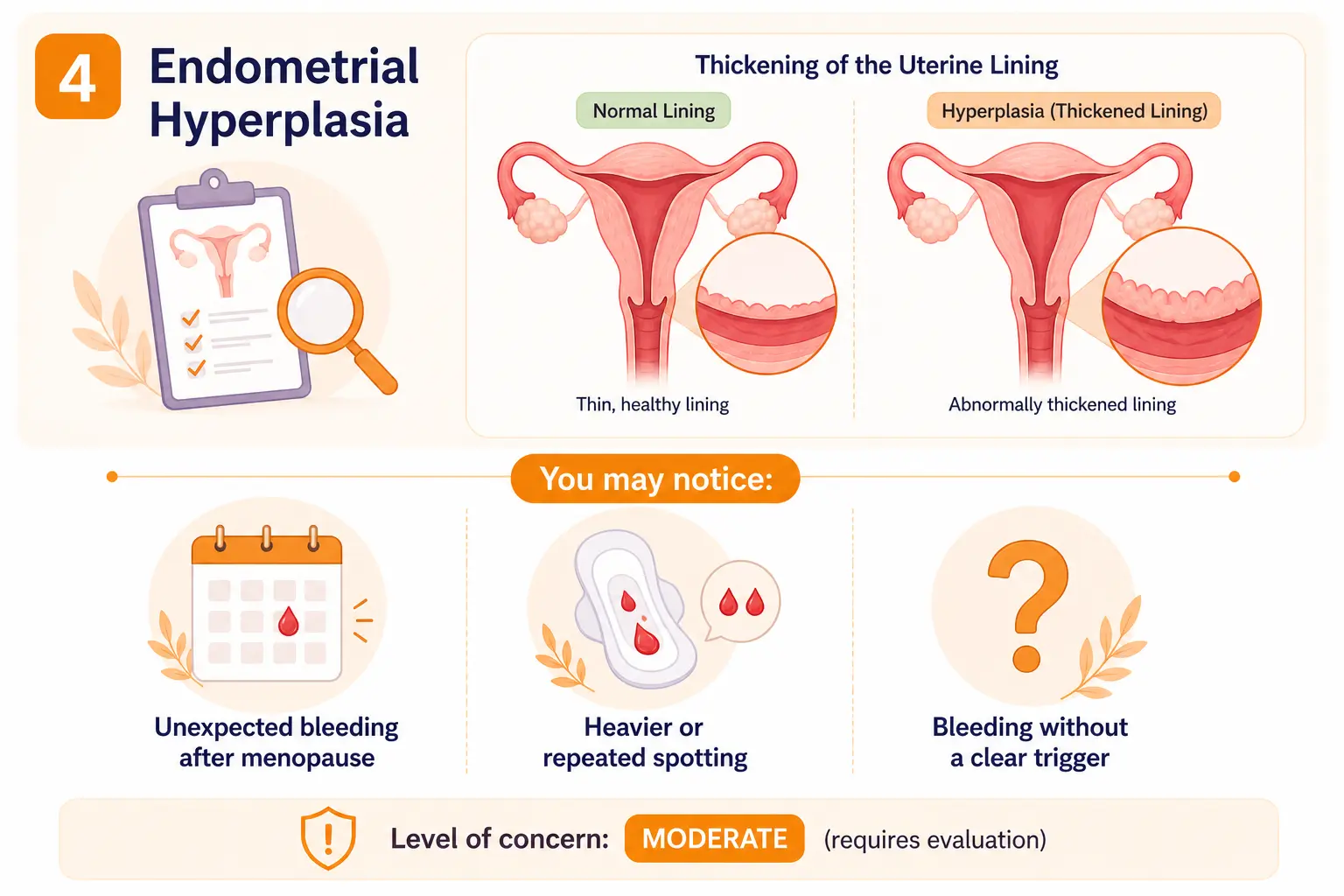
You may notice:
-
Unexpected bleeding after menopause
-
Heavier or repeated spotting
-
Bleeding without a clear trigger
Level of concern: 🟠 Moderate (requires evaluation)
5. Endometrial (Uterine) Cancer
In a smaller number of cases, bleeding after menopause may be linked to endometrial cancer. It’s important to note that this is less common, and many women with symptoms have non-cancerous causes.
Early detection plays an important role in effective treatment.
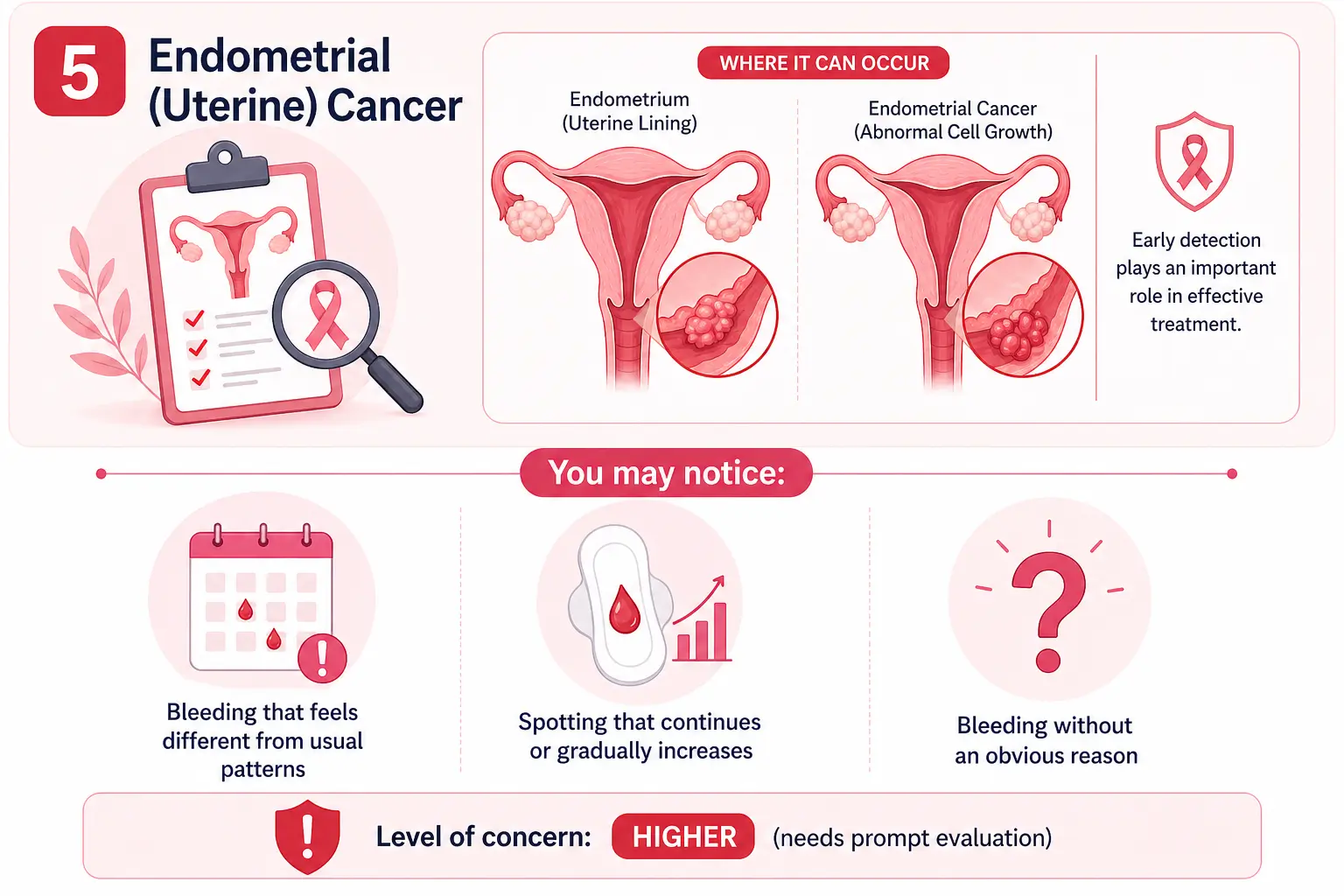
You may notice:
-
Bleeding that feels different from usual patterns
-
Spotting that continues or gradually increases
-
Bleeding without an obvious reason
Level of concern: 🔴 Higher (needs prompt evaluation)
6. Other Possible Causes
Less commonly, bleeding after menopause may be related to infections, cervical conditions, irritation, or certain medications such as blood thinners.
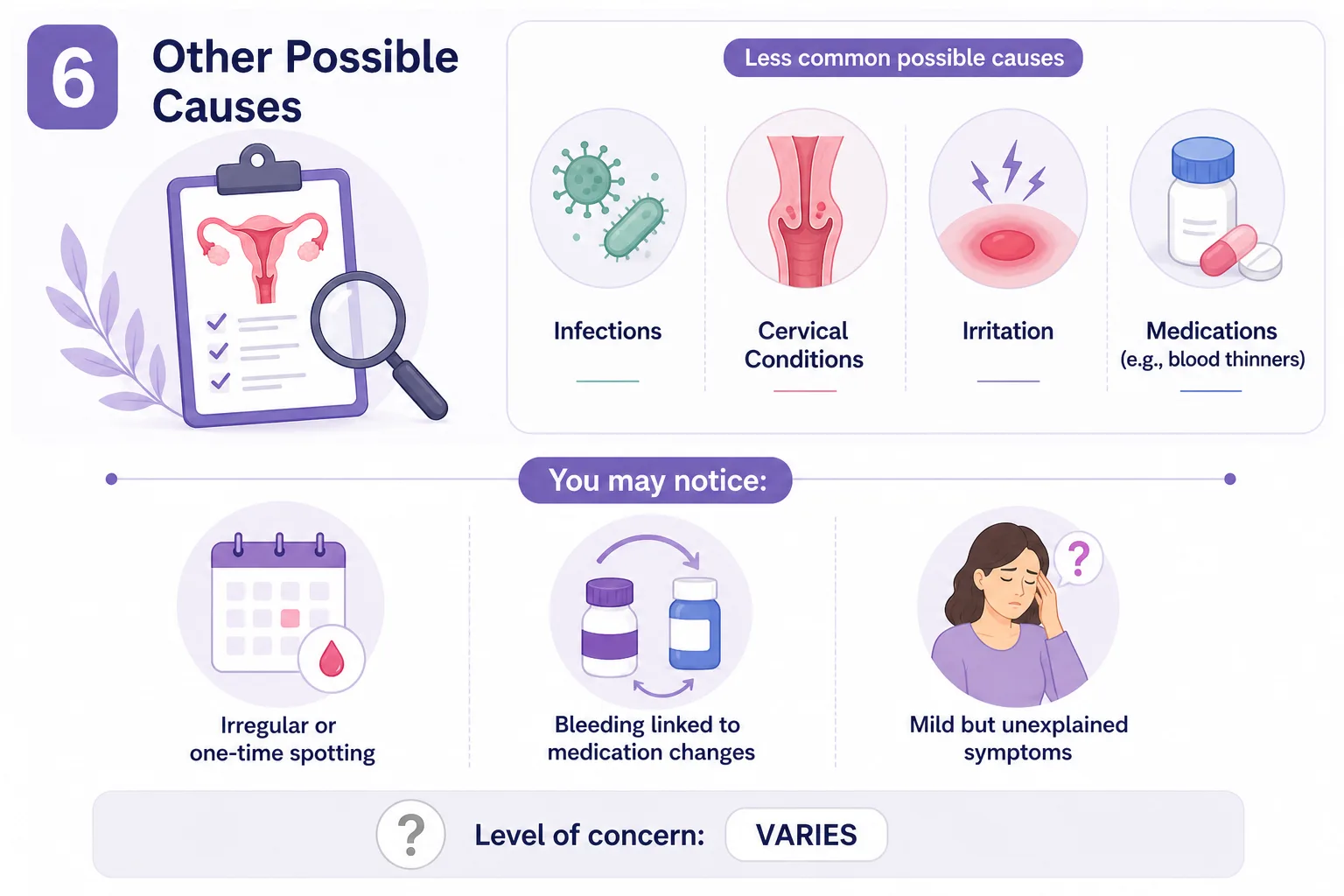
You may notice:
-
Irregular or one-time spotting
-
Bleeding linked to medication changes
-
Mild but unexplained symptoms
Level of concern: ⚪ Varies
Common types of bleeding after menopause include:
-
Light spotting – small amounts of blood or staining on underwear
-
Brown vaginal discharge – often older blood leaving the body
-
Pink or red discharge – may indicate more recent bleeding
-
Bleeding after intercourse – often linked to tissue sensitivity
-
Heavier or period-like bleeding – less common but noticeable
|
When Should You See a Doctor for Bleeding After Menopause?
Any bleeding after menopause should be evaluated by a healthcare provider, even if it happens only once or seems very light.

You should seek medical advice if:
-
You notice any spotting, staining, or bleeding after menopause
-
The bleeding occurs even as a one-time episode
-
You experience bleeding after intercourse
-
The bleeding repeats, persists, or changes over time
-
It has been months or years since menopause and bleeding appears again
Seek more urgent care if:
-
The bleeding is heavier than expected
-
You feel dizziness, weakness, or unusual fatigue
-
The bleeding starts suddenly and feels significant
Final Thoughts
We hope this guide has helped you better understand bleeding after menopause and what to look out for.
If something still feels unclear, don’t hesitate to ask, reach out, or book a consultation. It’s always better to have clarity than to keep guessing.
Share on Social Media
Loved what you read? Share this blog with your friends on X, LinkedIn,
or WhatsApp and spread the knowledge.














 Meet Your Doctor
Meet Your Doctor

Leave a Comment